Introduction
Sleep is not merely rest -- it is a hormonal production factory. During deep delta-wave sleep, your body produces growth hormone, repairs tissues, consolidates memories, and critically, synthesizes steroid hormones including progesterone. When sleep is fragmented or shallow, this entire hormonal assembly line grinds to a halt.
Delta Sleep-Inducing Peptide (DSIP) is a naturally occurring neuromodulatory peptide discovered in 1977 that promotes exactly what its name suggests: delta-wave sleep. Unlike sedatives that knock you unconscious, DSIP appears to optimize sleep architecture -- increasing the proportion of restorative deep sleep where hormone production peaks.
For progesterone specifically, the connection is straightforward. Progesterone synthesis is highest during quality sleep, and DSIP promotes exactly the kind of sleep where this synthesis thrives. In this article, you will learn how DSIP interfaces with sleep-based hormone production, what the research shows, and how FixMyT can help you understand whether sleep disruption is undermining your progesterone status.
Understanding Progesterone: The Protection of Your Metabolism
Progesterone occupies a unique position in the FixMyT metabolic tree at Level 4: Androgen Expression. Its role is protection -- acting as a counterbalance to estrogen, supporting thyroid function, and providing neurological calm through its neurosteroid properties.
The Progesterone node reflects these protective functions:
- Anti-estrogenic effects: Opposes estrogen's proliferative actions
- Aromatase modulation: Helps regulate estrogen production
- Thyroid support: Enhances cellular sensitivity to thyroid hormones
- Neurosteroid production: Metabolites like allopregnanolone calm the nervous system
When progesterone is low, the symptoms often manifest as anxiety, sleep disturbances (a vicious cycle), estrogen dominance symptoms, and impaired stress resilience. Many people do not realize that poor sleep itself may be both a cause and a consequence of low progesterone.
The upstream connections matter: Cortisol (at Level 3) suppresses progesterone, and poor sleep elevates cortisol. This creates a downward spiral where bad sleep leads to high cortisol, which suppresses progesterone, which then further disrupts sleep.
What Is DSIP?
Delta Sleep-Inducing Peptide is a naturally occurring nonapeptide first isolated from rabbit cerebral venous blood during electrically induced sleep. It was identified by Swiss researchers Monnier and Schoenenberger in 1977, who named it for its most prominent observed effect.
Key characteristics of DSIP:
- Sequence: Trp-Ala-Gly-Gly-Asp-Ala-Ser-Gly-Glu (9 amino acids)
- Molecular weight: 848.81 g/mol
- Research status: Limited human studies, primarily preclinical
- Administration: Subcutaneous (100-300 mcg before bed)
- Half-life: 15-25 minutes, though effects persist for hours
What makes DSIP unique is that it does not act as a sedative in the conventional sense. Rather than forcing unconsciousness, it appears to modify sleep architecture -- increasing delta wave activity during slow-wave sleep stages. This is the sleep phase most associated with physical restoration and hormone production.
For the complete technical profile, see the full DSIP profile on PepGuide.
How DSIP Supports Progesterone Function
The relationship between DSIP and progesterone operates through several interconnected mechanisms centered on sleep quality and stress modulation.
1. Delta Sleep Enhancement
DSIP specifically promotes slow-wave sleep (Stage 3 and 4 NREM sleep), characterized by delta wave activity on EEG. This is the sleep stage where:
- Growth hormone secretion peaks
- Cellular repair is most active
- Steroid hormone synthesis is optimized
- Cortisol reaches its lowest point
By increasing the proportion and quality of delta sleep, DSIP creates the optimal hormonal environment for progesterone production. Research in Neuropsychobiology demonstrated measurable increases in delta wave power during NREM sleep following DSIP administration.
2. Cortisol Modulation
DSIP has demonstrated significant effects on the stress axis:
- Attenuates HPA axis response under stress
- Reduces excessive cortisol output
- Normalizes disrupted circadian cortisol rhythms
- May modulate ACTH secretion patterns
This cortisol-modulating effect is particularly relevant for progesterone. Recall the "pregnenolone steal" phenomenon: when cortisol demand is high, pregnenolone is diverted away from progesterone synthesis. By reducing cortisol signaling, DSIP may indirectly preserve the pregnenolone pool for progesterone production.
3. Circadian Rhythm Restoration
Natural DSIP concentrations follow circadian patterns, peaking during nighttime hours. Exogenous DSIP may help restore normal circadian signaling in those whose rhythms have been disrupted by:
- Shift work
- Chronic stress
- Blue light exposure
- Aging-related changes
Restored circadian rhythm supports the normal pulsatile release of hormones, including those in the progesterone pathway.
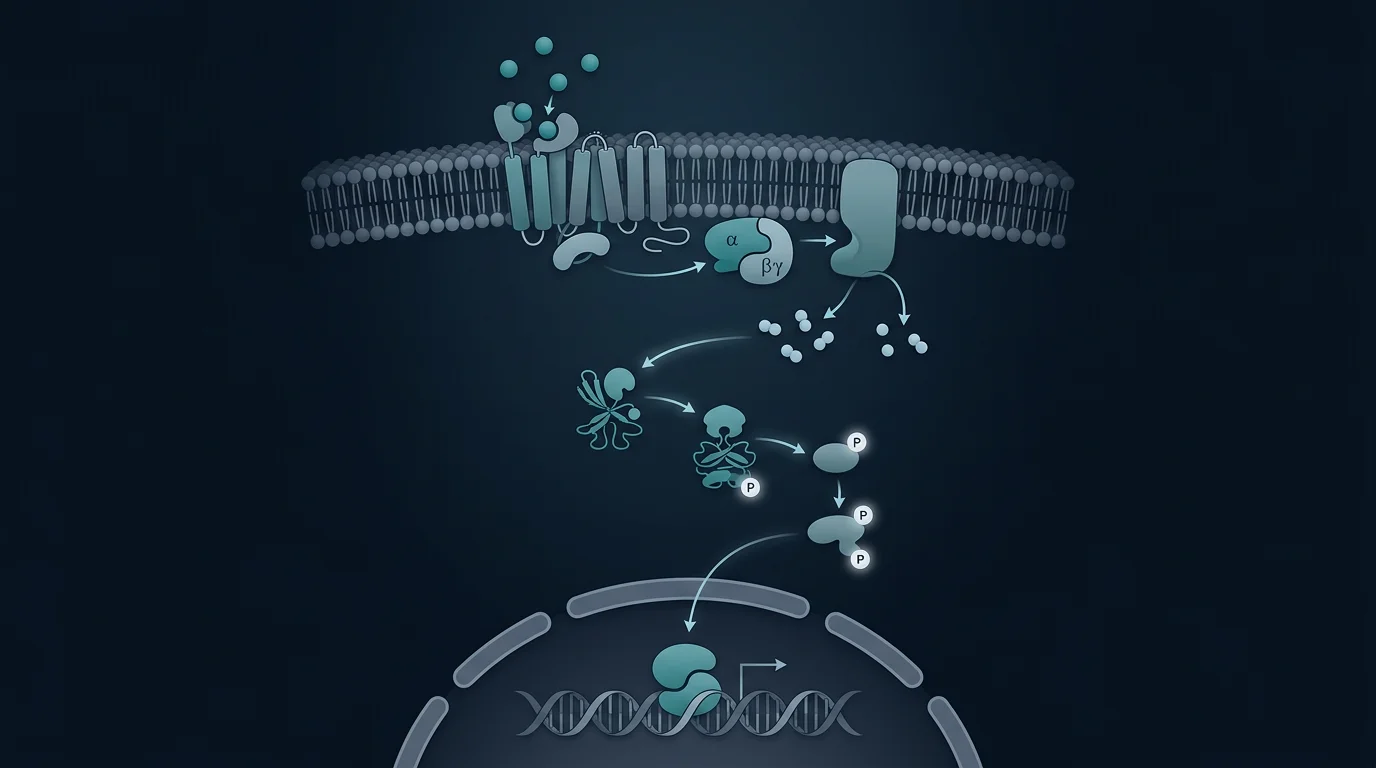
4. Endocrine System Modulation
Beyond sleep and cortisol, DSIP has shown effects on broader endocrine function:
- May potentiate nocturnal growth hormone release
- Some evidence of effects on gonadotropin secretion (LH/FSH)
- Influences met-enkephalin levels in the brain
- Possible effects on thyroid hormone patterns
These broader endocrine effects suggest DSIP may support hormonal health through multiple pathways, with sleep quality being the primary driver.
What Real People Are Saying
The peptide research community has shared experiences connecting DSIP use with improved sleep and hormonal markers:
"DSIP has completely changed my sleep quality. I'm getting into deep sleep faster and staying there longer according to my Oura ring. After about 8 weeks, my morning cortisol is down and interestingly my pregnenolone has come up on labs. Makes sense if the sleep is reducing stress demand." -- u/sleep_hacker on r/Peptides
"Using DSIP 200mcg before bed every other night. The sleep is noticeably deeper -- I wake up actually refreshed instead of groggy. Haven't measured progesterone directly but my anxiety has improved and I feel like my hormones are more stable overall. Less reactive to stress." -- u/endocrine_optimizer on r/Nootropics
"Ran DSIP for a month and got labs before and after. Sleep quality was significantly better. Cortisol:DHEA ratio improved. The interesting thing is my total T and free T both came up about 15% -- I'm attributing that to better sleep and lower cortisol allowing the whole system to work better." -- u/hormonelab_tracker on r/Testosterone
These are anecdotal reports and individual experiences vary. However, the consistent theme of improved sleep leading to better hormonal markers aligns with the established science of sleep-hormone relationships.
Monitoring Your Progesterone Health with FixMyT
Sleep quality and hormonal health are deeply interconnected. FixMyT offers a systematic way to assess whether sleep disruption is affecting your Progesterone node and overall metabolic function.
The FixMyT symptoms quiz evaluates indicators relevant to sleep-hormone connections:
- Difficulty falling or staying asleep
- Waking unrefreshed despite adequate sleep duration
- Afternoon energy crashes
- Anxiety and poor stress resilience
- Signs of hormonal imbalance despite normal-appearing labs
The visual metabolic tree shows how multiple factors affect progesterone production. Cortisol at Level 3 directly impacts Progesterone at Level 4, and sleep quality affects cortisol. By mapping your full metabolic picture, you can identify whether sleep intervention is a high-priority target.
For those researching peptides like DSIP, FixMyT provides context about whether sleep optimization is likely to yield hormonal benefits in your individual case.
Research and Considerations
The research on DSIP is intriguing but limited. Much of the clinical work occurred in the 1980s and 1990s, with the peptide's extremely short half-life presenting challenges for pharmaceutical development.
What the evidence supports:
- DSIP increases delta wave activity during NREM sleep (demonstrated in multiple studies)
- Sleep quality affects hormone production including steroids (well-established)
- DSIP modulates cortisol and HPA axis function (shown in preclinical and limited human studies)
- The peptide is well-tolerated with a favorable safety profile
What needs more research:
- Direct measurement of progesterone changes during DSIP protocols
- Long-term effects on steroidogenic pathways
- Optimal dosing for hormonal versus sleep-focused outcomes
- Head-to-head comparisons with other sleep interventions
The extremely short plasma half-life (15-25 minutes) is notable -- despite this, physiological effects persist for hours, suggesting downstream signaling or tissue-level effects that outlast the peptide's presence in circulation.
Disclaimer
This article is for educational and research purposes only. DSIP is not approved for human use by the FDA or other major regulatory agencies. Nothing in this article constitutes medical advice or a recommendation to use any substance.
If you are experiencing sleep disorders, anxiety, or symptoms of hormonal imbalance, consult with a qualified healthcare provider. Established sleep hygiene practices, cognitive behavioral therapy for insomnia (CBT-I), and addressing underlying medical conditions may be more appropriate first-line interventions.
Any decisions about health interventions remain your responsibility in consultation with appropriate medical professionals.
Learn More
- Full DSIP Profile on PepGuide - Complete technical details, dosing protocols, and safety information
- Pinealon for Neuroendocrine Balance - Another peptide supporting circadian and hormonal function
- FixMyT Metabolic Assessment - Understand your sleep-hormone connections
- Epitalon for Circadian Support - Complementary peptide for sleep and longevity
References
-
Monnier M, Schoenenberger GA. "Characterization, sequence, synthesis and specificity of a delta EEG (sleep) inducing peptide." Experientia. 1977;33:548-552.
-
Schneider-Helmert D, Schoenenberger GA. "Effects of DSIP in man. Multifunctional psychophysiological properties besides induction of natural sleep." Neuropsychobiology. 1983;9:197-206.
-
Graf MV, Kastin AJ. "Delta-sleep-inducing peptide (DSIP): a review." Neuroscience & Biobehavioral Reviews. 1984;8(1):83-93.
-
Kovalzon VM, Strekalova TV. "Delta sleep-inducing peptide (DSIP): a still unresolved riddle." Journal of Neurochemistry. 2006;97(2):303-309.
-
Leproult R, Van Cauter E. "Role of sleep and sleep loss in hormonal release and metabolism." Endocrine Development. 2010;17:11-21.
